Cross-Border Health Risk Assessment Tool
Travel Risk Assessment
Based on WHO guidelines and IHR regulations, determine if you should be screened at border crossings.
Your Risk Assessment Result
When you fly from Berlin to New York, or drive across the border from Mexico into Arizona, you might not think about health checks. But behind the scenes, a complex system is working to stop diseases before they spread. This isn’t science fiction-it’s the cross-border health coordination system built by the World Health Organization (WHO) and used by 196 countries. It’s the reason airports screen for fever, why border agents ask about symptoms, and why health data moves fast between nations during an outbreak.
How the System Was Built
The current system started after the 2003 SARS outbreak. That virus spread quickly across continents because countries didn’t share information fast enough. In response, the World Health Assembly agreed on the International Health Regulations (IHR) in 2005. It took effect in 2007, and since then, every country that signed on has been legally required to build basic health defenses at airports, seaports, and land crossings-called Points of Entry (PoEs).
These aren’t just fancy checkpoints. They’re the frontline. If a person with mpox shows up at a border crossing in Serbia, the staff there must detect it, notify their national health agency within 24 hours, and alert WHO. That’s not optional. It’s written into Annex 1A of the IHR. And it’s not just about viruses. The system also handles chemical spills, radiation leaks, and even bioterrorism threats.
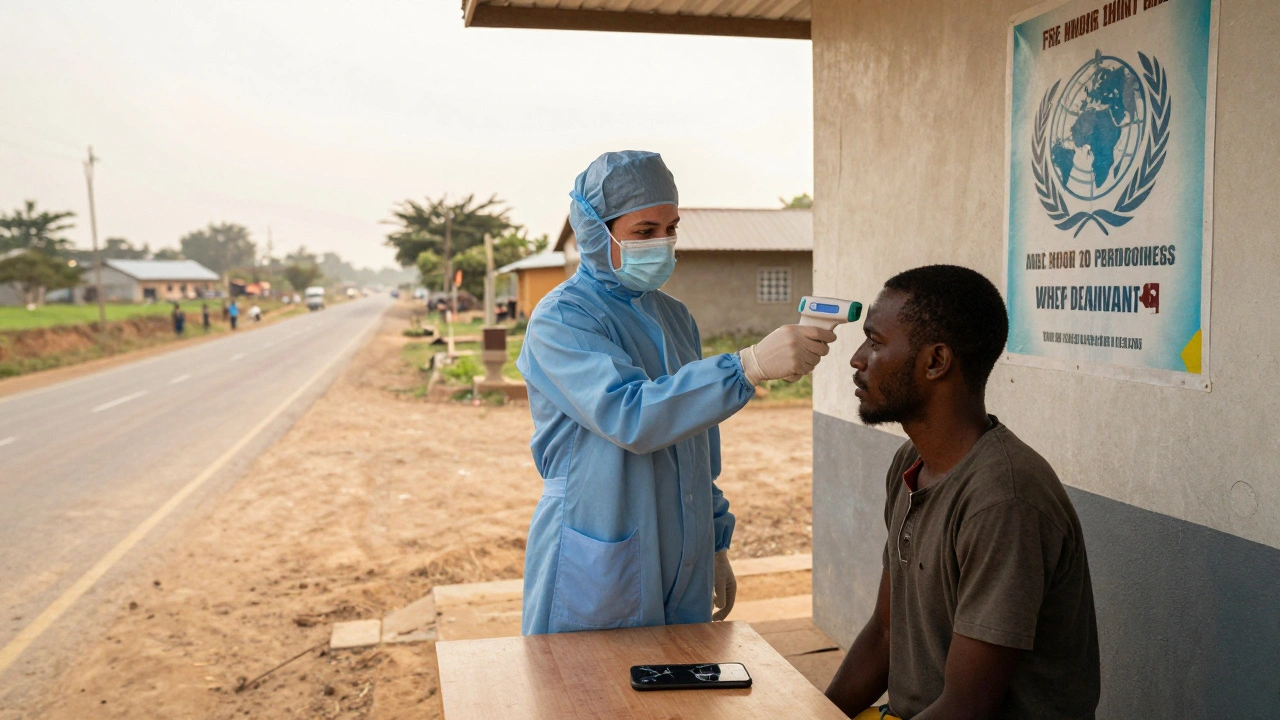
What Happens at a Point of Entry
Not every border crossing is the same. Big international airports have thermal cameras, health declaration forms, and isolation rooms. But at rural land borders? That’s where things get shaky. According to WHO’s 2022 assessment, only 52% of ground crossings meet full capacity requirements. Airports? Around 78% are doing okay.
At a working PoE, you’ll find:
- Staff trained to spot symptoms like rash, fever, or vomiting
- 24/7 access to medical care for travelers who fall ill
- Direct phone lines to national health authorities
- Systems that send data to the national surveillance network within hours
- Signs in multiple languages telling travelers what to do if they feel sick
And it’s not just health workers involved. Customs officers, immigration agents, transportation staff, and even local police all need to know their role. If someone is flagged as a risk, the border agency can’t just turn them away-they need to coordinate with health teams to isolate and test safely.
Data Sharing: The Hidden Backbone
What makes this system work isn’t just the physical setup-it’s data. When a case of measles is confirmed in Ukraine, that information must reach Poland, Romania, and Hungary within hours. That’s why the IHR requires countries to have real-time communication links with neighbors.
But here’s the problem: only 47% of ground crossings had formal agreements with their neighboring countries as of 2022. That means in many places, there’s no clear phone number to call, no shared email system, no agreed-upon format for sending data. One country might use paper forms. Another uses a digital portal. Without standardization, delays happen-and delays cost lives.
That’s why workshops like the one in Thessaloniki in November 2023 matter. Thirty-nine health officials from the Western Balkans met to fix exactly this. They didn’t just talk-they mapped out shared contact lists, tested emergency alerts, and agreed on common language for reporting cases. These aren’t nice-to-haves. They’re the difference between containing an outbreak and letting it explode.
Travel Protocols: When to Stay Home
Travel restrictions are controversial. People hate them. But sometimes, they’re the only tool that works.
In January 2024, WHO issued new guidance for mpox. It didn’t say “ban all travel.” It said this: “Persons with suspected or confirmed mpox should refrain from non-essential travel.” That’s a targeted, science-based protocol. It doesn’t shut down borders. It tells people who are sick: stay home. It also tells border staff: if someone has a rash and fever, ask about recent contact with infected people or travel to outbreak areas.
These protocols aren’t random. They’re based on how the disease spreads. Mpox isn’t airborne like COVID-19-it needs close skin contact. So banning flights won’t stop it. But asking travelers to self-report symptoms? That works.
And it’s not just about stopping sick people. It’s about preventing panic. Clear rules mean travelers know what to expect. Signs at airports say: “If you have a rash or fever, tell a health officer.” No guessing. No fear.
Why Some Countries Struggle
It’s easy to blame poor countries. But the issue isn’t just money-it’s coordination. In many places, the health ministry doesn’t talk to the transportation ministry. The border police don’t know what the local clinic can do. There’s no shared database. No joint drills.
WHO’s 2020 Handbook for Ground Crossings lays out the full checklist: communication systems, training schedules, emergency plans, public awareness campaigns. But implementing it? That’s where things break down.
Take a small town on the Congo-Rwanda border. There’s no running water at the checkpoint. No electricity for a thermometer. No internet to send data. The staff are overworked. They’ve never been trained on mpox symptoms. And they don’t have a phone number to call in Rwanda.
That’s not an outlier. It’s the norm in many low-resource settings. The IHR says every country must have these systems. But it doesn’t give them the tools to build them. That’s why regional support matters. The European Union funded the Thessaloniki workshop. WHO sent experts. Neighboring countries shared templates for health forms. That’s how change happens-not by mandate, but by partnership.
What’s Next?
The system isn’t perfect. But it’s getting better. WHO is now running simulation exercises in Africa, Asia, and Latin America. Countries are starting to share digital dashboards. Some are linking border health systems directly to national EHRs (electronic health records).
The big goal? Sustainability. As Professor Christos Hadjichristodoulou said in Thessaloniki: “We need to build a network that lasts beyond funding cycles.” That means training local staff-not just foreign experts. Making health coordination part of standard border operations, not a special emergency task.
And it’s working. After the 2023 workshop, three Balkan countries launched joint patrols at their shared crossings. They now check travelers together. They share data in real time. They’ve held three drills since November. That’s the future: not isolated borders, but connected health networks.
What You Can Do
You might think this doesn’t affect you. But it does. When you travel, you’re part of the system. If you’re sick, don’t fly. If you’re exposed to a known outbreak, tell a health official. Don’t hide symptoms. Don’t assume someone else will handle it.
And if you’re not traveling? Support policies that fund global health security. These systems don’t run on goodwill. They need funding, training, and political will. The next pandemic won’t wait for borders to catch up.





